Childhood Diabetes and Its Common Misconception as a Lifestyle-Related DiseaseSummer camps supporting children who endure prejudice

Key Points
- Diabetes is an ongoing health condition where your blood sugar levels are higher than normal as a result of limitations in the body’s capacity to produce or use insulin to reduce blood sugar levels. It is often misconceived to be the result of poor lifestyle choices or other factors.
- The Japan Association for Diabetes Education and Care runs summer camps for children with diabetes. The camps help the children make friends with other children living with diabetes, and to learn about topics such as diet and exercise.
- It is important to foster understanding in society in order to ensure that children living with diabetes do not develop a negative mentality toward their condition.
Insulin is a hormone secreted by the pancreas to regulate blood sugar levels. Diabetes is an ongoing condition where limitations on the body’s capacity to produce or use insulin cause continuously high blood sugar levels that may result in complications.
A survey published in 2021 by the International Diabetes Federation estimated that there are approximately 11 million people living with diabetes in Japan.*
The commonly used word for diabetes in Japanese is tonyobyo, which can be literally translated as “sugar-in-urine disease.” There is a movement calling to change this to the term daiabeteisu, the katakana Japanese phonetic spelling of the English word “diabetes.” It is argued that the term tonyobyo does not accurately reflect the disease’s symptoms, given that the presence of sugar in urine is not a criterion for diagnosing diabetes, and also that many adult patients are uncomfortable with the term due to the unclean associations that can be made with the character for “urine.”
Children who have developed diabetes at a young age also tend to suffer due to a lack of understanding from those around them. There are said to be cases in which children are unable to join their classmates for school lunch duty because they have to go to the nurse’s office before lunch to measure their blood sugar levels and inject themselves with the required amount of insulin. Some children are even teased if they have to eat a snack to supplement blood sugar levels when they drop too low.
They begin to feel the emotional strain of not being able to enjoy the same daily lifestyle as their classmates.

The Japan Association for Diabetes Education and Care (JADEC; external link, in Japanese) runs summer camps that provide such children with the opportunity to make friends with other children living with diabetes, and to learn about diet, exercise, measuring blood sugar levels, and other aspects related to managing one’s health when living with diabetes.
We spoke to JADEC board member Yasuko Uchigata about the kinds of difficulties faced by children who live with diabetes.
Diabetes: continuously high blood sugar levels that present the risk of complications
The Nippon Foundation Journal Editing Department: Could you start by summarizing what diabetes is?
Yasuko Uchigata: When we eat a meal, the stomach and small intestine break the food down into the energy source glucose, which is absorbed by the small intestine, increasing the levels of sugar (amount of glucose) in the blood. The pancreas instantly secretes the hormone insulin, which signals the liver and muscles to absorb the glucose so that it can be used as energy.
However, if for some reason the insulin does not function properly, or the very production of insulin declines or is almost non-existent, the blood sugar levels increase. Diabetes occurs when blood sugar levels remain persistently high.

Journal: What kinds of factors cause diabetes?
Uchigata: Diabetes can be divided into two main types according to the different causes of onset: Type 1 and Type 2 diabetes.
While its causes are still unclear, Type 1 diabetes is said to result when someone with a genetic predisposition to diabetes has an autoimmune reaction to a viral infection or other such trigger, destroying insulin-producing cells in the pancreas. The medical care that is currently available cannot provide a complete cure or prevent the destruction of insulin-producing cells.
On the other hand, Type 2 diabetes results from high blood sugar levels slowly developing, often without one realizing, due to various genetic factors related to limited insulin function combined with environmental factors such as overeating and lack of exercise.
- Reference: “What Kind of Disease Is Diabetes?”, The Japan Diabetes Society (external link, in Japanese)
Journal: What happens when blood sugar levels remain consistently high?
Uchigata: There is a risk that continuously high blood sugar levels will cause various symptoms or complications. Consistently high blood sugar levels generate distinctive symptoms including thirst, excessive urination, weight loss, and tiring easily. When high blood sugar levels continue persistently, the blood vessel walls in the microvessels are damaged, leading to hardening of the arteries.
When a thick blood vessel is damaged, there is high risk of complications such strokes or heart attacks, and when comparatively fine blood vessels have been damaged, there is an increased risk of developing retinopathy (eye disease), nephropathy (kidney disease), or neuropathy (nerve disease), which can also be described as the three major microvascular complications of diabetes.
It also causes various complications, such as a higher risk of catching infection or susceptibility to cataracts or periodontal (gum) disease.
Journal: What kinds of treatment methods are there for diabetes?
Uchigata: Diabetes is not the kind of disease with a simple cure — it is not possible to just take a medicine that reduces high blood sugar levels, for instance. People with diabetes need to manage and regulate their own blood sugar to follow target levels set according to factors such as age, and whether or not there are complications.
Type 1 diabetes is handled primarily with insulin therapy, which entails supplementing the insulin that is lacking. This therapy can take the form of regular injections, generally three times a day, where blood sugar levels are measured before meals and the amount of insulin to be injected is determined depending on the amount of food that will be eaten, or, the use of an insulin pump, which continuously delivers insulin to the body.
On the other hand, Type 2 diabetes is treated by making adjustments to one’s diet and exercise routine with the aim of achieving a target blood sugar level. This may also be combined with insulin therapy.
For both Type 1 and Type 2 diabetes, the aim of treatment is to prevent or curb the complications that can result from persistently high blood sugar levels.
Camps that give children who endure prejudice towards their diabetes the chance to make friends also living with the condition
Journal: JADEC runs summer camps aimed at children with Type 1 diabetes. What prompted the launch of the camps?
Uchigata: Japan’s summer camps for childhood diabetes were first launched by pediatrician Hiroshi Maruyama in 1963, modeled on similar camps held overseas. JADEC took over the organization of the camps in 1967 and began public funding for the camps. While further developing the camps in each region, the camps are now run in 50 locations across Japan. Apart from during the COVID-19 pandemic, they have been held every year.
Since 2014, the summer camps have also been open to children with Type 2 diabetes.

Uchigata: As I just mentioned, diabetes is the kind of condition where self-management is crucial. One of the aims of the camp is therefore for the children to learn and become proficient in self-management, such as learning how to administer their own insulin shots and how to respond when blood sugar levels drop too low.*
The children also learn about topics such as how diet and exercise function in relation to blood sugar level, and get great exercise through physical activities such as mountain climbing or playing in the river.
An even greater aim of the camps is for the children to make friends with other children living with the same disease. Type 1 diabetes patients account for around 2% of all those with diabetes. The cases of onset are said to be high among very young children, but as the number of people with the condition is low, it is difficult to find fellow diabetes sufferers in everyday life. It is easy for children to develop a feeling of isolation, as they wonder whether they are the only one taking insulin injections and measuring their blood sugar levels.
However, at the summer camps for childhood diabetes, they are able to meet other children who are also living with diabetes just as they are, as well as adults with an understanding of their condition. When we ask the children what they enjoyed about the camp, the most common answer is meeting and becoming friends with other children living with diabetes.
- Blood sugar levels may drop too low if too much insulin has been injected, or less food has been eaten than planned. Initial symptoms are trembling hands or decreased concentration, while severe cases can be fatal.
Journal: JADEC and the Japan Diabetes Society jointly proposed the adoption of the term daiabeteisu — the katakana form of the English word “diabetes” — as the new naming of the disease in Japanese. Was this proposal also prompted by misconceptions of diabetes?
Uchigata: Yes, it was. The word tonyobyo (the commonly used Japanese term for diabetes) is associated with deeply rooted negative stereotypes of the disease as being the result of neglecting one’s health or lack of exercise. Not only children, but also adults living with diabetes suffer due to the lack of understanding among those around them.
There is also the fact that the term tonyobyo — literally, “sugar-in-urine disease” — does not accurately reflect the symptoms of the disease, given that in some cases diabetes can be diagnosed without the presence of sugar in the urine. The name may also evoke images of uncleanliness, due to the fact that it contains the kanji character for “urine.” We are therefore pursuing an advocacy initiative* (external link, in Japanese) to revise the Japanese terms that are used in connection with diabetes and reinvent the image of the disease.
- Initiatives aimed at safeguarding the rights of minorities and the socially vulnerable by acting as a spokesperson to assert their claims and appeal to those in politics, finance, society and other fields.
Journal: That makes sense. What other kinds of initiatives is JADEC pursuing?
Uchigata: We also organize seminars where our representatives visit schools to provide instruction for teachers. This was in response to feedback from schoolteachers worried that their limited knowledge of diabetes and inordinate concerns about what could happen to a student with diabetes if their blood sugar levels drop made them unsure what approach to take to such children attending sports classes or participating in school trips.
We believe that in order for children with diabetes to comfortably enjoy school life, it is important for not only the children, but also the teachers to be equipped with accurate knowledge of diabetes.
Journal: And we have heard that the summer camps have also been offered online since 2021. Is that right?
Uchigata: Yes. We had to put the camps on hold during the COVID-19 pandemic, but we drew on online resources to hold a virtual camp for children with diabetes (external link, in Japanese) to ensure that the children and volunteer staff did not drift apart.
We held a virtual camp in November 2023 as well, where the children were able to use the virtual environment to enjoy activities such as mountain climbing games, group discussions, and a drawing contest.
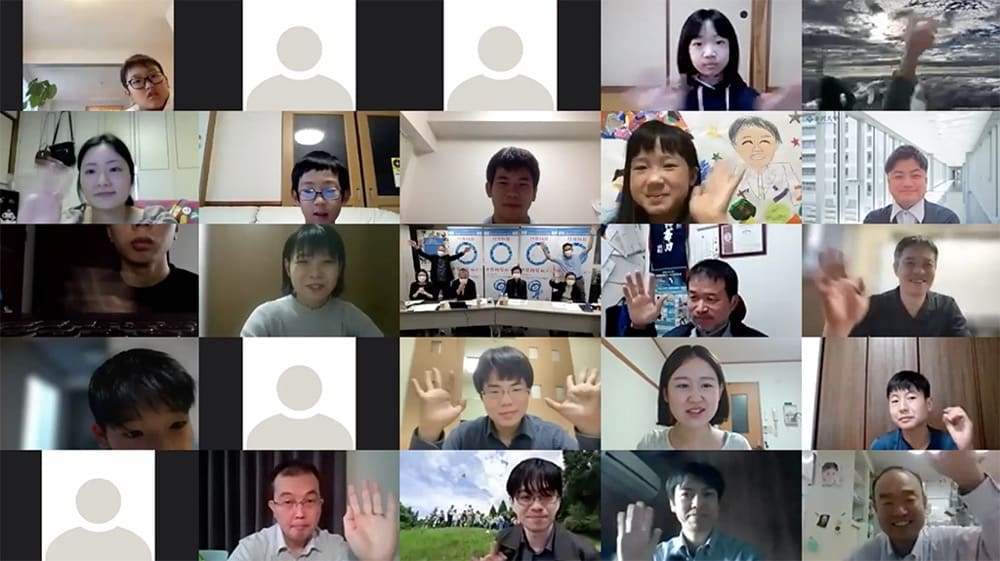
Journal: What was the response of the children?
Uchigata: At the in-person camps, children were only able to mix with other children from their local region. The virtual camps, however, gave the children the possibility to enjoy interacting with children above and beyond their local environments. For instance, a child from Fukuoka in the south of Japan could quickly make friends with a child from Hokkaido in the far north. Another aspect of the virtual camps that made a strong impression was the fact that hospitalized children were also able to take part.
Since 2023, about 60% of the in-person camps around Japan are back up and running, so we intend to continue to offer both in-person and virtual camps in the future.
Journal: The camps are such a wonderful initiative. Let us conclude by asking: what can we do as individuals to make our society comfortable for children with diabetes?
Uchigata: I think that what is most crucial is understanding diabetes correctly and eradicating prejudice. The last five or six years have seen a rising number of people openly living with diabetes in the public eye, such as Minoru Iwata, a former baseball player for the popular professional baseball team the Hanshin Tigers, and I think that the correct perception of diabetes is gradually spreading across society as a whole.
However, negative stereotypes and other misconceptions are still strongly rooted. I think that we still have a little way to go before we have a society in which children can live openly with their diabetes. We at JADEC will also do our best to pursue initiatives to promote greater understanding.
Journal: What needs to be done to create such a society?
Uchigata: I once heard the professional wheelchair tennis player Tokito Oda* saying “para sport is more fun.” I think that children with diabetes also need an older role model — someone who has come to terms with their circumstances and pursues a successful career at the same time.
- Tokito Oda developed bone cancer at the age of 9. After battling his illness, he took up wheelchair tennis and, at the age of 14 years and 11 months, became the youngest player in history to top the junior world ranking. He is 17 years old as of January 2024. Reference: “A Candid Chat with Tokito Oda: The Youngest Professional Wheelchair Tennis Player in the History of Parasport”, Parasapo Web by The Nippon Foundation Para Sports Support Center (external link, in Japanese)

Uchigata: An older role model can show children that living with diabetes is nothing to worry about and that everything will be fine as long as they carefully manage their condition. I would also like the children to believe for themselves that diabetes is nothing to be ashamed of.
I think that the predisposition to Type 2 diabetes may have developed in ancient times as a means for us to survive periods when food was lacking. A physical constitution in which insulin does not function properly developed in order to allow the body to draw energy from even the smallest amount of food, and such genes were passed down through the generations.
It is also said that it is thanks to the fact that many humans possessed such genes that humanity was able to prosper for so many years. I would like people who live with diabetes to be able to believe that diabetes is not a disease to be ashamed of.
Editor’s Note
This interview prompted us to notice our own subconscious prejudice that diabetes is a condition affecting people who fail to properly manage their health.
To ensure that no children or patients suffer from prejudice toward diabetes, we need to advocate the adoption of a new, more appropriate term for diabetes in Japanese and help to ensure that more people across society as a whole have a correct understanding of diabetes.
Text: The Nippon Foundation Journal Editing Department
Photo: Eizaburo Sogo
Profile
Yasuko Uchigata
Yasuko Uchigata was born in 1951 and is a board member of the Japan Association for Diabetes Education and Care. She has dedicated great efforts to treating, researching, and raising awareness regarding diabetes, in her roles that include director of the Tokyo Women’s Medical University Adachi Medical Center (now the Adachi Medical Center) and director of the university’s Diabetes Center. She has published several books on the topic, including Shoni/yangu tonyobyo — Nobinobi shikkari sapoto (“Diabetes in infants and young people: Easygoing yet thorough support”)





